The beginning...
Diagnosis & Testing:

7/19/2016-- The Call. In March of 2016, I was visiting my uncle in Seattle, when I felt a lump near my armpit one night while taking a bath. I didn't think much of it at the time, and life continued on for about 4 months. By that time, the lump was much bigger and had become increasingly more painful. I ended up having to put an ice pack on it in the evenings, when it hurt the most. I went for an ultrasound in July and it puzzled the radiologist. She said it was "one of the weirdest things I've seen." At first glance, they thought it was an in-grown hair, but that was soon ruled out because it didn't appear to have any attachment to the surface of the skin. I was relived to hear them say that it had no blood flow, because that ruled out cancer in my brain. I felt my first sense of worry when they ordered a biopsy immediately. I went outside, called my mom and then Stew, to let them know I was a little confused about the findings. After about an hour, I went for the biopsy. I consented to a study that would use a few pieces of the biopsy tissue to study cancer, (at that time, it wasn't believed that I did have cancer, but I had to consent to this test upfront because they needed to extract 3 or 4 extra samples to send to the research group). There were 3 or 4 resident students who came in to observe the procedure. Duke is a teaching hospital, so there were always residents around. I got a few shots of local anesthetic before they inserted the biopsy needle, several times. That was pretty painful. There are lots and lots of nerve endings near the armpit, so unfortunately, I felt a lot. One of the residents attempted to distract me by talking and asking me questions, but it didn't help. It was not fun. I would later read that there is a very small chance that doing a biopsy of a tumor can actually shake some of the cells loose and cause the cancer to spread.
The next morning, the doctor's office called and left a voice mail asking me to come into the office at 3pm to get my results. I thought that was kind of weird. It was 9 in the morning and I just wanted to know then. I called them back and told them to tell me over the phone, I wasn't waiting all day and then driving over there. The woman asked me more than once to come in and after I declined, she responded by saying the doctor would call me back ASAP.
Not 15 minutes later, the phone rang. "I don't have good news for you." She called it invasive adenocarcinoma with ductle metaplastic features. At that moment, it didn't mean too much. When she said "You have cancer," my whole body started shaking. It was the most terrifying moment of my entire life.
Out of complete fear, I asked her if I was going to die. She had no answers. None.
On July 19, 2016, I was diagnosed with breast cancer at 31 years old.
7/26/2016-- The Waiting Game. It continued to get worse when I couldn't get scheduled to see a doctor for 8 days. Somewhere around 170 hours of my brain's refusal to shut off. I had to close my eyes to go to sleep 8 times. I didn't know if I was going to live or die. Night time was the most difficult. During the day, I would ebb and flow between helpless terror and everything's going to be alright. Night time was not so easy. There was nothing except me and my thoughts. It will chill you to the bone to play scenarios in your head of your loved ones going on without you, when you feel like you're right in the middle of creating the life you've always wanted. Having confirmation that your life is in danger and that fixing it may be beyond control, is hands down, the worst type of emotion I've ever known. I didn't even know it existed before this. Your friends and family try to comfort you, but you're still staring death right in the face.
The next morning, the doctor's office called and left a voice mail asking me to come into the office at 3pm to get my results. I thought that was kind of weird. It was 9 in the morning and I just wanted to know then. I called them back and told them to tell me over the phone, I wasn't waiting all day and then driving over there. The woman asked me more than once to come in and after I declined, she responded by saying the doctor would call me back ASAP.
Not 15 minutes later, the phone rang. "I don't have good news for you." She called it invasive adenocarcinoma with ductle metaplastic features. At that moment, it didn't mean too much. When she said "You have cancer," my whole body started shaking. It was the most terrifying moment of my entire life.
Out of complete fear, I asked her if I was going to die. She had no answers. None.
On July 19, 2016, I was diagnosed with breast cancer at 31 years old.
7/26/2016-- The Waiting Game. It continued to get worse when I couldn't get scheduled to see a doctor for 8 days. Somewhere around 170 hours of my brain's refusal to shut off. I had to close my eyes to go to sleep 8 times. I didn't know if I was going to live or die. Night time was the most difficult. During the day, I would ebb and flow between helpless terror and everything's going to be alright. Night time was not so easy. There was nothing except me and my thoughts. It will chill you to the bone to play scenarios in your head of your loved ones going on without you, when you feel like you're right in the middle of creating the life you've always wanted. Having confirmation that your life is in danger and that fixing it may be beyond control, is hands down, the worst type of emotion I've ever known. I didn't even know it existed before this. Your friends and family try to comfort you, but you're still staring death right in the face.
7/27/2016-- My Very First Doctor's Appointment. I had a big sense of relief knowing that I was being treated at Duke University Hospital in Durham, NC. It's a world-renowned medical center and I was confident that I'd get good care there. I met my surgeon this day; Dr. Georgiade. He's a pretty old guy who can't hear too well, but apparently his father helped establish Duke, so their family has a long history with the hospital. Everyone there raved about how he's top notch in his field. His nurse "Old Dee," was just so great. She had me crying and laughing, then gave me a big comforting hug before I left. That was my first moment of relief since the call. Stew called her Oldie, but Goodie. The doctor ordered the first of my MRI's to see what we were dealing with. He noted that he didn't feel anything in my lymph nodes, which was good news, but only the tests would be definitive. I didn't know then, but I would soon be diagnosed with what my oncologist believed to be stage II (or possibly III) breast cancer.
Dr. Georgiade gave me 3 great pieces of advice, that I'd end up carrying with me every day of this process:
1. Prepare for a marathon, not a sprint.
2. Be selfish with your time and energy.
3. Swallow each new piece of information one at a time.
FYI: Lymph nodes act as filters that collect fluid and waste materials that are outside the blood stream. They are important for cancer patients, because doctors have a better idea of whether or not the cancer has metastasized (spread to other areas) based on the presence or absence of cancerous cells within the nodes. Read more about lymph nodes: http://www.cancer.org/cancer/cancerbasics/lymph-nodes-and-cancer
7/29/2016-- Meet and Greet With My New Oncologists. I met with a geneticist and sent some DNA to the lab to sequence 4 specific genes for mutations; BRCA1, BRCA2, PALB2 & TP53. Mutations on these genes are thought to be linked to breast cancer. This was relevant for me because there is a strong history of breast cancer in my family (my mom and her sister). The results came back negative, which we thought was a little strange, since my mom and aunt both had breast cancer (a combined 4 times). The geneticist said they still believe my cancer is genetic, however, not linked to these genes. Perhaps the genetic link results from a mutation on a gene that's not yet discovered to be linked? I'm not sure about that. A positive result to mutations on these genes could've indicated that I may be at higher risk for things like ovarian cancer, other types of breast cancer, melanoma, pancreatic cancer, etc. The negative result indicated that I'm not necessarily at higher risk for those types of cancer.
Next, I met with my radiation oncologist, Dr. Horton. She also did not feel anything in the lymph nodes and mentioned that I'd most likely need 4-6 weeks of daily radiation after surgery. She noted that since the cancer is on my right side, my heart would be safe from the radiation and that was a huge relief. I lost touch with her after that appointment, as she did not come into play until much later in my journey.
Lastly, I met with my medical oncologist, Dr. Kimmick. At this stage of the game, Dr. Kimmick ordered my port placement, 12 rounds of weekly chemotherapy and then 4 rounds of bi-weekly chemo. Then I'd have 2-3 weeks off to heal, surgery then possible radiation. I originally planned to work through all of this (who can afford not to?). I was in good spirits after these appointments, I felt a lot more informed and ready to get started with my treatment plan. After so many sleepless nights, I finally slept through the night.
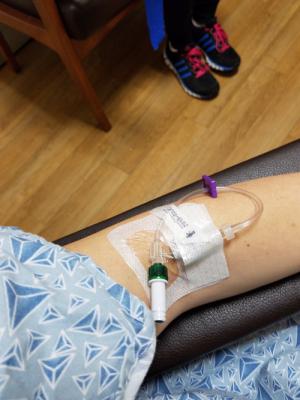
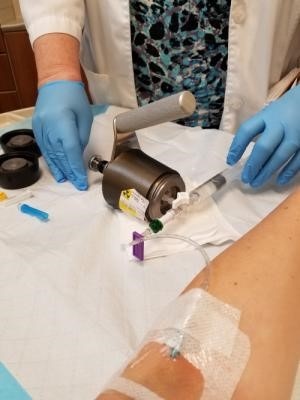
8/1/2016-- Let The Testing Begin. My day started with an MRI, which shows the doctors if the cancer has spread from the breast tissue into the lymph nodes. The MRI machine clicks really loud, so you get to listen to music during the test, to drown out the noise. The pictures require an infusion of dye, so that was my first time getting an IV catheter inserted for that purpose (2 pictures below). The test lasted about 25 minutes, piece of cake.
Before I could get out the door to head home, I got a call that my EKG and echo-cardiogram could be completed immediately. I had to go back to the lab to have a blood draw and then headed to the cardio unit. The EKG and echo took about 20 minutes. I was told my heart looks good. The tech was great, she cooperated with my curiosity and answered all my questions.
EKG vs. Echo-cardiogram
EKG (electrocardiogram)- a test used for measuring the electrical efficiency of the heart. It displays the rhythm of the heart and can detect abnormalities, i.e., beating too fast or too slow.
Echo-cardiogram- a more advanced test that uses ultrasound to create a visual image of the heart. It helps doctors view the internal structure of the heart and how well blood is able to flow through it.
To read more about the heart tests: www.vistacollegepro.com/healthcare/ekg-technician/what-is-the-difference-between-an-ekg-test-and-echocardiogram/
8/4/2016-- PET CT Scan. PET scans use radioactive isotopes to detect cells in the body that are dividing abnormally fast, like cancer cells. Before the test, you get an injection of sugar + radioactive material. Since cancer cells tend to be more active than normal cells, cancer cells absorb more of the sugar substance to carry out their cellular processes. This causes them to take up more of the radioactive material which "lights up" during the scan. This gives doctors an indication of areas which may be of concern and from there the doctor can do a biopsy to determine whether or not the cancer has spread. One of the downsides to this test, is that tumors have to be a specific size before the scan can pick them up, so even if your PET scan comes back looking clear of spread, it's not definitive.
Side note: This was my first unpleasant experience; there was a malfunction of the pieces of the catheter the nurse put in my arm and blood was leaking all over. I'm never woozy at the sight of blood, but she had to throw me back in the chair because I almost passed out. It was also my first experience with contrast (during the CT). It feels like a really warm rush of fluid inside your body that goes from your head to your toes. It took an hour for the isotope to circulate, but the scans only took about 25 minutes.

8/5/2016-- PET CT Scan Test Results (Big Deal). This day I met with my medical oncologist. She was pleased to tell me that my PET scan was clean and there was no indication the cancer had spread. She also changed up my chemo schedule a little. She decided to start me on Cytoxan and Adriamycin in a week and have infusions every other week, instead of every week. I was relieved to have an extra week to recover. Her plan is to watch how the tumor responds after the first few treatments and decide to keep up with those two drugs, or switch up, if necessary. I was able to get a bunch of appointments scheduled and have a chemotherapy "class" on Monday. I felt anxious to get some information on what to expect and even more anxious to get started with treatment! I had my first infusion in my arm and plan to have my port placed and ready for the second infusion. I was feeling exhausted from so many long days at Duke, but also positive and confident in my doctors.
8/8/2016-- Chemotherapy Class. Rewind to yesterday: went to the gym with Stew and was feeling totally fine. After 2 minutes on the elliptical, I had to get off, because I didn't feel right. I decided to walk instead. I got through my walk fine and then went to lift some weights. I hadn't been to the gym in about 2 weeks, since I was busy at Duke, so I grabbed a few lighter weights, knowing it was going to be a little rough. When I began struggling with the light weights, I felt the tears well up in my eyes, because I realized that this was the beginning of a long, strenuous journey that I didn't want to take. So as I sat in the corner, feeling upset and sorry for myself, Stew comes over and just as he always does, he put everything into perspective for me. He reminded me that I'm going to have to hold myself to a different set of expectations for the next several months and that's just what it is. He started rattling off a list of things I can do besides weights, so that I don't have to feel disappointed every time I get into the gym. He is the epitome of "tough love," and that is exactly what I needed. There have been a few times since this diagnosis where I can't help but think of how this is just so unfair, total bullshit and just not what me (or anyone) needs or wants. Stew is so good at picking you up and dusting you off. He pushed the pity feelings out and helped me focus on what I had to do. I had no choice, but to deal with this head on and just get better. That's all there is to it.
So, about chemo class, I met with the pharmacy specialist (D0nna Topping) at Duke, to explain my treatment in detail and answer all my questions. This lady was so amazing. She spent an hour and a half telling me all of the "what to expects". She set me up with this nicely organized calendar reminding me what to take and when to take it. She explained every medication, what it does, and gave me so many preventative suggestions on how to deal with all the side effects of my chemo. I felt much more ready to start my chemo in a few days. I noticed myself doing things a little differently. Knowing my hair would soon be gone, I kept catching myself looking in the mirror and washing it just a little bit longer. I smiled at people more. I started to listen better. Songs had totally new meanings. The regular stresses of life had become so negligible. I knew that with school starting soon, my plate, which was already overflowing, would become even fuller, but it didn't worry me. I wasn't sure if my brain was just fried, or if I was still in shock, but I just felt like my only care in the world was to take this treatment and be as strong as I possibly could to get through it and get it over with.