Treatment:
chemotherapy
8/12/2016-- Chemo 1 of 8. All chemo days went a little like this:
1. To the lab for a blood draw
2. To the oncologist's office for check up
3. Upstairs to the 4th floor for treatment
As long as my blood counts were high enough, I was allowed to have chemo that day. Before chemo could be administered, I was always given oral anti-emetic meds and an IV drip of anti-emetic meds. It took about a half an hour or so before we could ever get the chemo infused. Since my first chemo was going into a vein in my arm, this day became a spectacle. The sweet nurse couldn't find a vein and after a few unsuccessful needle sticks, she ended up having to use the "vein viewer." Once she was able to get a good vein in my middle left forearm, she manually pushed in the Adriamycin, which was a bloody red color. I didn't notice any weird symptoms, except my urine was red as the meds were flushed out of my body. The Cytoxan came from a drip and caused a weird burning sensation in my nose (they call it wasabi nose). These 2 chemos took about 45 minutes total. I also had to get a Neulasta patch after every chemo. This fabulous invention gets placed on treatment day and then injects its medicine exactly 27 hours later (when needed). It boosts your white blood cells, which are damaged by the chemo.
Med List for Chemo 1-4:
Decadron (Dexamethasone) 4 mg--steriod/anti-inflammatory
Zofran (Ondansetron) 8 mg--anti-emetic
Emend (Aprepritant)--anti-emetic
Ativan (Lorazepam) 0.5 mg--anti-anxiety
Neulasta (Pegfilgrastim) 6 mg--bone marrow stimulant
Zoladex (Goserelin) injection-- Estrogen suppressant
Decadron, Zofran & OTC Claritin were taken days 2-4 following chemo to relieve nausea and help with bone pain.
Letrozole (Femara) 2.5 mg-- Aromatase inhibitor/estrogen suppressant, would be added to my med list following radiation therapy and would continue with Zoladex for 5 years.
Noted side effects: Chest tightness, shortness of breath, extreme exhaustion and chemo brain. (Chemo brain would end up causing me to take disability for nearly 6 months)
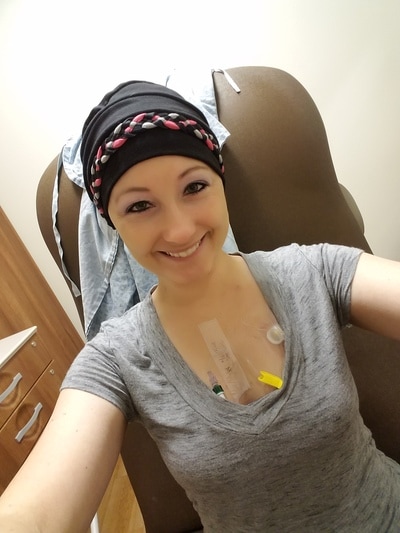
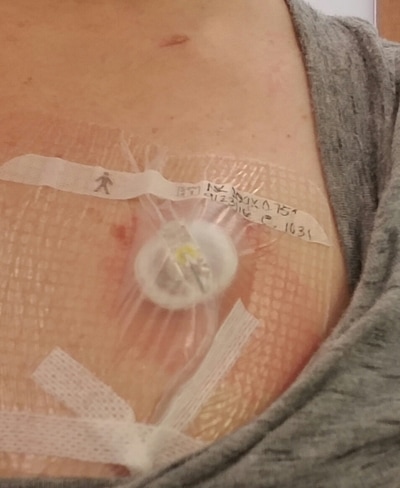
8/17/2016-- Port Placement. Chemotherapy drugs are very toxic and can cause damage to small veins, like the ones in your arms. A port allows chemotherapy (and other meds, like your pre-chemo meds) to be injected right into a large vein which leads directly to the heart. This allows the drugs to be diluted by the blood stream and more evenly and efficiently distributed to the body. You also get your blood drawn from your port, so your veins aren't exposed to so many pricks; which can cause scarring and damage.
On the morning of my port placement, the nurse could not stick my vein to give me my anesthesia. I remember telling him that I was going to pass out if he didn't get it soon and next thing I knew, I was waking up to him still trying to access a vein. This was probably the worst experience I had through this whole process. I started sweating and felt like I was going to throw up. Luckily, Stew and his mom were there and told him to stop. He was unable to get my medicine going, so I was taken back for the procedure, where the anesthesiologist was able to easily access my vein to administer the anesthesia. They used some sedation, but I was still awake do remember quite a bit. I could see what they were doing on the monitor. It was kind of interesting, I could see all my ribs and the catheter tube moving around. They used an ultrasound and an MRI machine to track the catheter and direct it to the right vein. The port ended up being a GREAT accessory and definitely made life easier.
This day taught me how important it is to advocate for yourself. You are entitled to ask for a different nurse if the one who's trying to stick you just can't find a vein. Even better idea? Ask for an anesthesiologist! I noticed that they were pros at finding and sticking without much pain.
8/26/2016-- Chemo 2 of 8. I had my port accessed for the first time. I loved my port because it made blood draws and chemo so much quicker and less painful. The only negative aspect to my port was that it was painful if I moved my arm the wrong way and sometimes, the port would get smashed in my chest. That seemed to happen a lot during the night, which was kind of painful. Also, after a couple weeks, I developed a blood clot in the catheter, which became problematic.
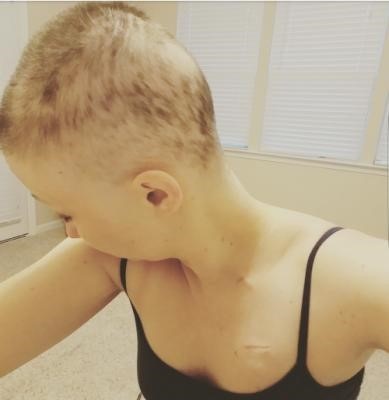
I had already begun cutting my hair short in preparation of losing it all. While sitting in the waiting room, exactly 14 days after my first chemo infusion, I noticed that my hair started to fall out. Every time I ran my fingers through my hair, a lot of hair came out right into my hand.
Overall, I had a GREAT day at Duke. My labs and oncol appointment were on time, minimal waiting. Since I didn't have to get chemo through my arm this time, I saw a nurse who accessed my port for the first time. She was awesome and knowledgeable and funny....Ms. Polly. I used some numbing cream (Emla), so I barely felt the prick.
From there, we went to the oncologist's office and saw a few nurses. Not much to report from them, general questions and procedures. They did note that my blood counts were high enough to go ahead with chemo for the day, so that's what we did.
Upstairs on the chemo floor, we got stuck waiting for a while, but overall, we started at 8am and ended around 1pm, so I'm calling that a win. Prior to chemo, I started with my normal regimen of several oral anti-nausea meds. Along with that, an IV drip of my strong anti-nausea. Those had to process for a half hour and then chemo could begin. Just like last time, the nurse had 3 big syringes of Adriamycin, which she slowly pushed into the line. After that, my IV drip of Cytoxan. I was REALLY groggy and sleepy during the chemo, I blame the meds she gave up front. I don't remember being that way last time, but Stew said I was, so? After the chemo, I got my Neulasta auto-injector placed on my stomach, and also had to get a shot of Zolodex in my stomach. Zolodex essentially shuts down my ovaries, in order to try and preserve my eggs. This was probably the most painful part of today, because a big needle is needed to puncture a hole for a metal rod to be inserted which delivers the medication as a slow release "pellet."
I officially started losing my hair exactly 2 weeks after my first round of chemotherapy. I noticed that my head was sore over night while laying on my pillow. I thought it may have been from wearing my wig earlier that night, but it may have had something to do with this sudden loss of LOTS of hairs. I was washing it in the sink and noted both hands full of hair. It had been pulling out in little clumps all day.
Noted side effects: terribly painful hiccups, dry mouth, and blisters in my mouth, numb pinky toes, severe pain and then numbness in my right arm/hand, random bouts of shortness of breath and some pretty severe chest pain/pressure. I also lost my taste for coffee after 15 years! My oncologist said using metal utensils may cause weird taste issues. I also noticed major hair loss, scalp pain & tenderness, exhaustion, CHEMO BRAIN so bad. I also had a noticeable shrinkage in the size of the tumor!
A few days later.........
9/9/2016-- Chemo 3 of 8. Since I mentioned my severe chest pain as a side effect, my nurse Christy, ordered an EKG and echocardiogram to check for heart function and a chest CT w/contrast to check for a pulmonary embolism (blood clot in the lungs). I had to get these tests before she would allow me to get more chemo, so that added some time to my day. Everything ended up being normal, so chemo went as planned. They were swamped upstairs, so instead of my normal recliner chair, I got a bed. It was pretty great and everything went smoothly. :)
When I got home, Christy called and asked why I didn't get my echocardiogram. Um, oops? I guess I forgot. Chemo brain was by far my worst symptom. It seemed like I was moving in slow motion and my brain was just not working right. I already make a lot of lists, but I found myself having to write down the most basic things. My hair was pretty much gone by third chemo, but the oncologist said I wouldn't lose all of my hair until I started taking the second set of chemos.
9/23/2016-- Chemo 4 of 8. This day was full of extra "stuff." I left for Duke at 8am and didn't return home until 6pm. Long, tiring day.
It started with my echocardiogram, which was incredibly interesting. The tech answered and explained all my 5783 questions. I learned A LOT about my heart, veins, valves and arteries. She showed me everything she was doing. This test checks to make sure the blood is flowing properly through the heart. Later on in the day, I got confirmation that this test was normal.
I left that for the lab, to get my port accessed and my blood taken. That went pretty smoothly.
From there, I had to get a chest X-ray, since I was coughing from some kind of virus, so we had to rule out pneumonia before I could proceed with chemo. That test came back negative for pneumonia, so onward.
Next I had to meet with the oncologist, who was about 2 hours behind. (Annoying, but I get it). While waiting, I was able to get my flu shot. I also got my new calendar of chemo + drugs, since I would soon be switching from a double dose chemo to a single dose chemo. The new drug is call Paxitaxol (Taxol) and was a THREE HOUR INFUSION....ugh. The purpose of switching chemotherapy, is an attempt to minimize symptoms, while still maximizing effectiveness. A few pros of Taxol are: no more mouth sores and no meds for the 3 days following chemo. New potential side effects: more thinning/hair loss and peripheral neuropathy (numbness in fingers/toes... potentially permanent). I just hope, hope, HOPE the "chemo brain" symptoms dissipate.... at least a little. I have been struggling so much. The week after chemo was becoming worse and worse, but at least I had my second week without chemo, which I feel totally normal and I was able to function. I also noticed while waiting for 2 hours, that my port was itchy and burning a little. I may have left the numbing cream on too long that morning, which caused some kind of allergic reaction. So much so, that later on, the chemo nurse ended up removing the sterile dressing to check and make sure all the numbing cream had been wiped off my skin before I had chemo.
After being about 2.5 hours late for chemo, I was starving and had to get a bite to eat, so I checked in for chemo, then went to the food court. As soon as I returned and sat down, they buzzed me, so there was very little waiting there. We got started with all my anti-nausea pills and then my anti-nausea drip. I rolled my medicine dispenser out on to the rooftop garden they have at Duke. It was so perfect outside-- nice breeze, warm. I was able to sit without my hat comfortably. I had to go inside for the nurse to push the Adriamycin, but was able to go back out again for the second chemo, Cytoxan. I also had to get my Neulasta patch and it was time for Zolodex, so I got a lot of pricks today. My oncologist measured the tumor: Day 1, pre-chemo, it measured 5.5cm, today it measured 2.6cm. That. Is. Huge. News. Such a relief knowing that the chemo was doing its job.
10/8/2016-- Chemo 5 of 8. The day started with the normal lab draw to check my cell counts before chemo. Last time, I seemed to have developed an allergy to the numbing cream, which you put on your port so that you don't feel the needle prick. I tried once more and had a horrible itch. I ended up wiping it off after about 10 minutes and then stopped using it after that. Either way, the prick didn't hurt, so that was fine.
I went to see the nurse at oncology next. She said my counts were fine. I was low on one, but she let me go for chemo anyway. I was still sick with a virus. I had now been sick for 19 days! She looked in my ears and throat, said it seemed to be clearing up. I mentioned this weird thing that had been going on in my left arm for a few weeks, seemed like it had been going on for months. There was a section of my lower arm, near the bend of my elbow, but on the inside of the bend, that had been acting funny. One day I would wake up it would be bright red, the next day it would be bruised. The vein was hard and rubbery, it was painful but then the next day it would look totally fine. The nurse ordered an ultrasound to see what was going on there. Before the u/s, I had to go up for chemo. The new chemo regimen started: Taxol. I got a huge dose of Benadryl (50mg) IV drip, a dose of Pepcid and a dose of Decadron (steriod) before chemo, but didn't have to take any medicine at home, so that was a big plus! Taxol can cause a bad allergic reaction, so they give you Benadryl, just as a precaution. The fact that it came IV was like being hit with a brick. Literally, all at once, I felt it. The room started spinning and I had to close my eyes because it felt so awful. The Pepcid and Decadron help fight inflammation and any residual stomach issues (nausea). The chemo itself has a 3 hour infusion, so that was REALLY boring. I couldn't read or color or do much of anything because the Benadryl had me feeling loopy as hell and NOT in a good way. The chemo nurse said I can ask for a reduction in the dosage next time, since it caused such a dramatic reaction.
After chemo, we went to get the arm ultrasound. The tech started up in my neck and worked all the way down my arm looking at my veins and arteries. It was very interesting, on the screen you could see 2 black circles (one vein and one artery). She would push down with the handle of the ultrasound machine and one of the circles would flatten out and one would stay open. She said with compression, veins collapse, but arteries don't, so that's how you can tell which is which. Also, if there is a clot in a vein, it won't collapse, so that's how they can find clots. After she took nearly 60 pictures, she asked us to wait around while the pictures were read. After about a half hour she came back and said we needed to go back to the oncologist's office, because they found a clot in the spot that had been giving me issues. So... back upstairs we went.
In the oncol's office, she explained that the clot is in a superficial vein (very close to the skin and not a major vein). The normal treatment for thrombosis (clot) of this type of vein is heat, elevation and inflammatory meds (ibuprofen). She also said that since the subcutaneous vein is thrombosed, the ultrasound was unable to confirm that I did NOT have a deep vein thrombosis, which is life threatening, as it can lead to stroke or pulmonary embolism. Since it was 5pm on a Friday, she asked if I wanted to get on a blood thinner, just in case the deeper veins did have a clot, until I could be cleared on Monday morning. Even though the nurse and I both agreed that I most likely didn't have a deep vein thrombosis, since I wasn't having any swelling or issues with my hand on that side, I still couldn't get the idea of a stroke/pulmonary embolism out of my head, so I decided to play it safe and take the blood thinner until I could get a CT scan on Monday to rule out any issues with the deeper veins. The blood thinner is a syringe (Lovenox), I have to put in my belly x2 per day until my appointment Monday. I had a hell of a time giving myself the syringe. I was so scared that my hands would shake. The needle stick doesn't even really hurt, but the medicine burns! My poor belly was being all pricked up.
Med List for Chemo 5-8:
Benadryl (Diphenhydramine) 50mg IV drip to 25mg oral tablet-- antihistamine
Zofran (Ondansetron) 8 mg--anti-emetic
Emend (Aprepritant)--anti-emetic
Ativan (Lorazepam) 0.5 mg--anti-anxiety
Neulasta (Pegfilgrastim) 6 mg--bone marrow stimulant
Zoladex (Goserelin) injection-- Estrogen suppressant
10/21/2016-- Chemo 6 of 8. Nothing exciting to report, other than I had a HUGE breakthrough regarding my port. I had developed a sensitivity to tasting the saline flush, which seemed to have gotten worse over time. I dreaded the saline and asked the nurses to push it slowly to minimize the taste. I had tried sucking on altoids, mentos, lemon heads, holding a drink in my mouth, among other things. When the port nurse suggested plugging my nose, I couldn't believe I didn't think of it sooner. It totally worked and I didn't taste anything, so that was a big win.
My counts came back fine, a little low on the platelets, as usual, and elevated liver function this time, which is not my norm. She explained that it's probably the chemo and not a worry for now, it just needed to be monitored.
Chemo was fine. Instead of 50mg IV Benadryl, I got 25mg oral Benadryl, so that helped minimize symptoms a lot, but I still felt pretty crappy/sleepy/out of it for most of the afternoon. We sat outside for a little, but I didn't feel well enough to read or write thank yous or anything.
I met with the surgeon 2 days ago and had a lot of questions answered, but lots of new questions popped up. I'm fairly certain that I'm going to get a double mastectomy, with mom and aunt's history, there's no reason to do anything else. With this, comes the option of implants vs. using my own fat to create the new boobs. I would much rather use my own fat, because then I won't have to worry about my body rejecting it and I also won't have to go back for new implants every 10 years, or whatever the protocol is. Apparently, I was not a candidate for that at this time, but surgery can't even happen for 6 months after the completion of radiation, so that won't be until at least end of summer of 2017. I still had lots of questions. The 3 docs were planning to meet on 10/31 to discuss my case & provide some more information. I was feeling pretty defeated, as I was told I'd have to continue the painful stomach injections for at least 3 months post-surgery, which meant a minimum of 5 more months. Ugh. Not only were they painful, they were so expensive. Before insurance, they cost $1200 for a one month supply. Unbelievable.
I flew to Akron, to walk in the American Cancer Society's Making Strides Against Breast Cancer event. It was really great to be surrounded by my family and friends. I never thought I'd be walking one of those events as a current fighter! It was very humbling and uplifting.

11/7/2016-- Chemo 7 of 8. It was crazy to think that I only had to go through the routine ONE MORE TIME until I'd be done with chemo forever! Everything went fine at chemo. I even had some company. My dad & gramma drove down for "the cancer experience." They got to see the hospital and spent the day, sitting around with me for treatment. My only issue at oncology was an elevated liver function (apparently normal for chemo patients), but I had to have another CT scan to rule out anything non-chemo related, since we have "big decisions" coming up. Big decisions referring to surgery and what that would consist of. I had been trying to get a surgery date out of them for weeks, but that was unsuccessful. After chemo was over, the surgeon would order an MRI, then surgery would be about 4 weeks post-chemo. They have to give your body enough time to heal from chemo and be in tip top shape for surgery. I was having some stabbing pains in my legs which I attributed to the Taxol. I took at least 3 naps and I was feeling pretty tired and worn out, but otherwise ok.
My hair had still not completely fallen out, although my eye lashes started to. I had little stubbly hairs all over my head. They weren't falling out, but didn't seem to be growing either. It was like 2 day old guy beard stubble, but it had been that way for months. It seemed like it did actually grow a tiny bit, because I had noticed that it was painful when I laid my head down on my pillow.
Last issue to report: those stupid blood thinner shots!! I hated them so much, they were still so painful, however we did have a breakthrough. I had become terrified of giving myself the shot after the first few doses, so Stew had been doing them. One night, I was determined to do it on my own, so I did, and now I'm afraid to let him do it. haha, gahhhh. It is crazy how much your adrenaline pumps when you have to give yourself a shot!
11/19/2016-- Chemo 8 of 8. Chemo "Graduation" Day. (it's a real thing). This was the happiest I'd been since this whole process started. The longest, most detrimental, temporarily life changing part of this journey had come to an end. I was most excited for chemo brain to go away and to get my eyelashes back. I was also optimistic about being healthy for more than a 10 day stretch. Chemo went fine, zero issues to report.
The CT from 2 days prior was unremarkable, so no major issues with my liver function being elevated and no sign of any new cancer!
Next up: surgery. I had an MRI scheduled for the following Monday. This gave the surgeon a clear picture of what he would be dealing with. I saw him 11/30 to secure surgery plans & set a date within a week or two. I had to wait 4 weeks post chemo for surgery, so my body had time to heal. I did not want to wait a minute longer than necessary!